Scientists have developed a graphene patch that can monitor sugar levels in diabetic patients as well as deliver metformin – a drug used to treat diabetes – through the skin.
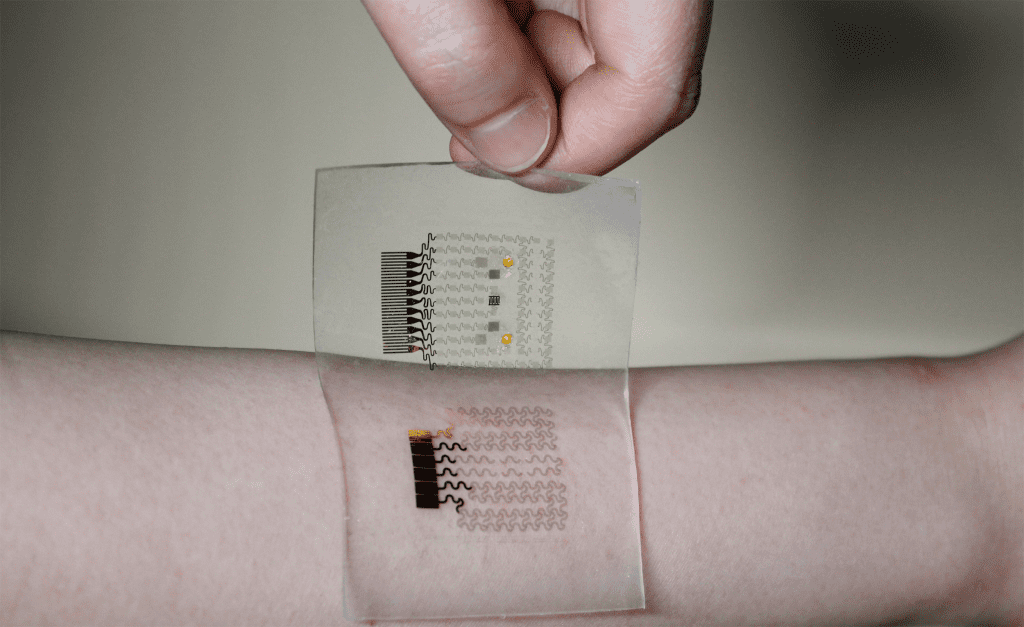
Credit: Hui Won Yun, Seoul National University
After being described only a few years ago, graphene is already starting to show its potential applications in medicine. Owing to its high carrier mobility, conductivity, flexibility and optical transparency, graphene is a versatile material in electronics. Graphene, the one-atom thick layer showed huge potential in biosensors, as it is flexible, conducts electricity, and can be transparent, soft and very thin.
However, the low electrochemical potential in graphene synthesized by chemical vapour deposition limits its application in biosensing. For this reason, Dae-Hyeong Kim from the Seoul National University in South Korea tried to upgrade it – with gold. Graphene doped with gold and combined with a gold mesh has significantly higher electrochemical qualities than bare graphene, sufficient enough to form a sweat-based diabetes monitoring and feedback patch. They demonstrated the technology in mice.
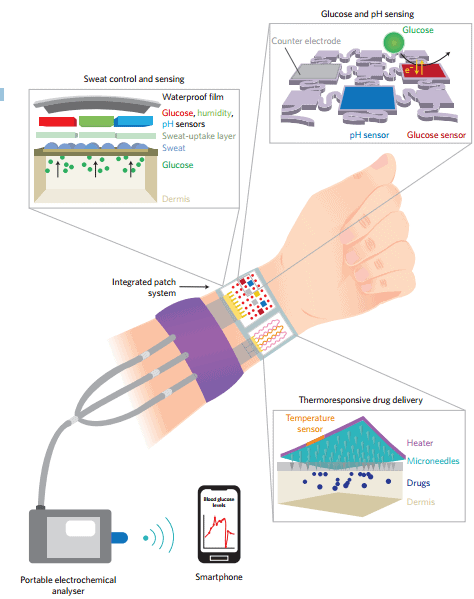
portable electrochemical analyser, which acts as a power supply and controller that wirelessly transmits data to a remote mobile device (such as a smartphone). Figure adapted from the Supplementary
Information for ref. 2, Nature Publishing Group
The patch contains a several sensors that monitor humidity, glucose, pH and temperature. It analyzes sweat to determine if an injection is needed. Because the enzyme-based glucose sensor is affected by pH changes in sweat, the pH and temperature sensors correct the glucose measurements by taking into account pH and temperature in real time, improving its reliability. If glucose levels are deemed unsafe, micro-needles dissolve their coat and release the drug metformin. You probably have to refuel it every few days, but otherwise, the entire process is automatic and painless. Until now, the process was invasive and potentially painful. In the accompanying News & Views article, Richard Guy from the University of Bath writes:
“The global increase in diabetes is a significant physical and economic burden. Reducing the pernicious morbidity of the disease requires the effective control of blood sugar levels through a strict regimen of diet and drug treatments (for example, insulin injections). At present, glucose levels in the blood or interstitial fluid (the solution that bathes the tissue cells) are monitored by either ‘finger sticks’ — a procedure in which a finger is pricked using a lancet to obtain a small amount of blood for testing — or the insertion of sensors through the skin.”
Of course, everything will have to be scaled up for human use, but this is a big step in the right direction. Guy continues:
“Although the holy grail of diabetes management — a non-invasive feedback system combining glucose monitoring and responsive drug delivery — is not yet at hand, Kim and co-workers have certainly moved the field closer to this coveted prize.”
DOI: 10.1038/nnano.2016.38
Was this helpful?