Most organs in the adult human body are capable of regeneration, which means they renew their cells to keep the tissue healthy and functional. This capacity is enabled by adult stem cells, which are present in most organs and divide to create new cells that replace older, damaged ones.
It turns out these stem cells can be isolated and grown in the lab. When we do this, the stem cells form tiny replicants of the organs from which they were extracted, which we call “organoids”.
Alongside our colleague Yorick Post, who recently moved from Utrecht to the Silicon Valley commercial sector, we’ve produced a human tear gland organoid, which we’ve been able to make cry organoid tears – not by being nasty, of course, but by subjecting the organoid to adrenaline, which is released in humans when they’re subjected to pain. By studying our organoid tears, we might be able to help develop treatments for dry eye disease, including by transplanting our organoids back into human patients.
Mini organs
Until recently, it was very difficult to study stem cells in the lab as they could not be cultured in a Petri dish. Then, in 2009, the perfect recipe was found to culture stem cells of the intestine, which grew into tiny replicates of the intestine: a mini organ. Because of this resemblance, we now call these in vitro models “organoids”.
Since then, most organs have been made in organoid form, used to study the physiology and illnesses associated with that particular tissue. More recently, organoids have been used to study how SARS-CoV2 affects different organs, finding that SARS-CoV2 could infect the human intestine, explaining why some patients with COVID-19 experienced diarrhoea.
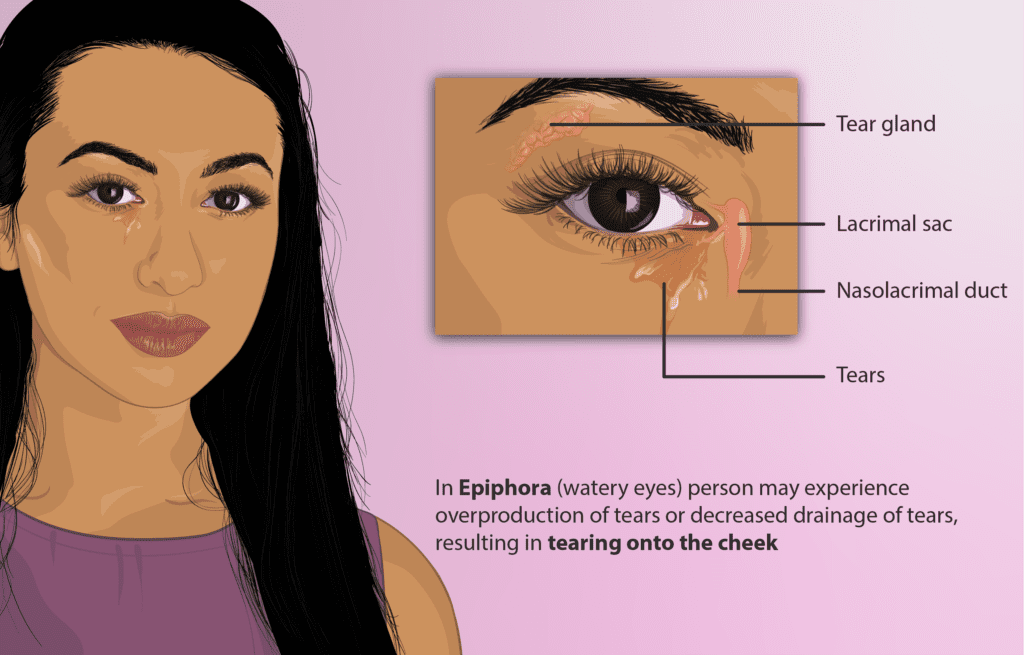
With more and more organs being created as organoids in the lab, we searched for an organ that hadn’t been considered yet: the tear gland. The tear gland is actually a very important organ: it produces the tears that lubricate the eye and protect it from infections.
When the tear gland doesn’t function properly, people experience itchiness and pain, a disease known as “dry eye”. This occurs in at least 5% of the adult population worldwide. Until now, studies of this disease were hindered by the lack of a good human tear gland model. We set out to establish one, by creating tear gland organoids.
Gland designs
To start an organoid culture, you need tissue directly from a patient. We obtained tear gland samples from the hospital and processed them into small pieces.
These pieces were placed in a droplet of gel, like a cushion. Importantly, this gel allows stem cells to grow in a three-dimensional environment, enabling them to organise into any shape. By stimulating the tear gland stem cells to divide, we made our culture grow. A few days later, we could actually see the first tear gland organoids in a dish, shaped like a sphere.
This was only the first step, as these tear gland organoids mostly contained stem cells. Tear gland stem cells are different from the mature cells that are present in the tear gland. Importantly, the stem cells themselves are not capable of making or shedding tears.
But tear gland stem cells do give rise to mature tear gland cells that are capable of crying. This process is called “differentiation”, and it takes place as soon as we stop stimulating stem cells to divide into other stem cells. We found it took at least seven days of culturing before our tear gland organoids could produce tears.
Tearjerkers
The final step in our experiments was to make our organoids cry. In humans, crying upon feeling pain is induced by stimuli such as adrenaline. To recreate this process in a dish, we exposed our tear gland organoids to adrenaline. Adrenaline made our tear gland organoid spheres swell like balloons. The organoids were secreting their tears on the inside: crying, but with nowhere for their tears to go.
What can now be done with these tear gland organoids? First, scientists can use them to study how the tear gland works: how it makes tears, what kind of tears it can make and what happens when the tear gland does not produce tears anymore.
At present, people with dry eye disease must constantly apply eye drops to lubricate the ocular surface. With tear gland organoids, scientists can now screen for better, more effective medicines that could help treat dry eye disease. Tear gland organoids could even eventually be transplanted back into patients with dry eye.
This strategy is already being applied in a clinical trial with salivary gland organoids. Patients treated by radiotherapy following head and neck cancers often lose their salivary glands, resulting in dry mouth. It’s hoped that transplanted salivary gland organoids could treat this affliction.
One other tissue we have our eye on is the tear gland of a crocodile – which is remarkably similar to human tear glands, but with some interesting differences. One day soon we may grow crocodile tear gland organoids in our lab, producing “crocodile tears” in the clinical environment of a Petri dish for the very first time.
Marie Bannier-Hélaouët, PhD Student, Hubrecht Institute, Utrecht University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
Was this helpful?



