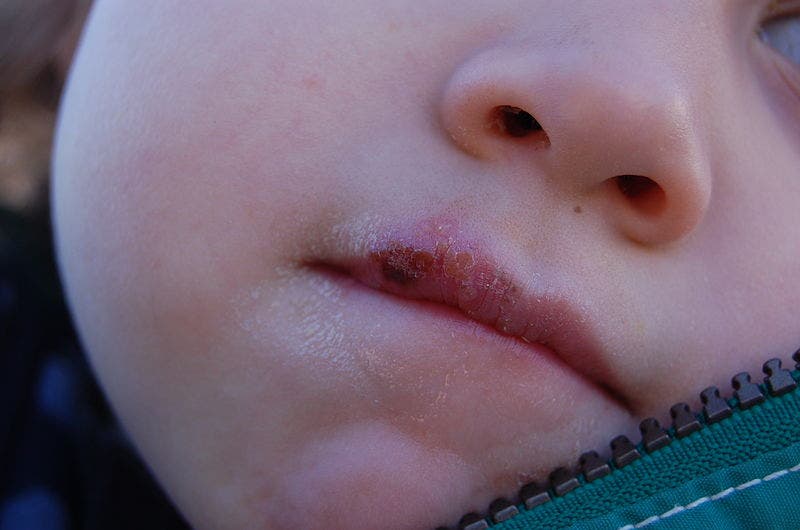
The herpes simplex virus represents a sore spot in more ways than one. Without a warning, a victim’s sores might flare up with no warning, triggered by factors as light as stress and exposure to UV light. Cold sores, also known as fever blisters, are one of the most common symptoms of herpes (HSV) reactivation.
Now, new research at least tells scientists what exactly goes on when the clinical Herpes simplex virus (HSV-1), one of the forms, reactivates. UVA Today notes that “the new insights help doctors better understand what is happening in neurons and the immune system,” and that could lead to ways to prevent unwanted outbreaks, the researchers hope.
What do we mean by one of its forms? According to the World Health Organization, herpes simplex virus-1 (HSV-1) is one of two herpes simplex virus germs. The other is herpes simplex virus type 2 (HSV-2). WHO draws an important distinction between the two.
“HSV-1 is mainly transmitted by oral-to-oral contact to cause oral herpes (which can include symptoms known as ‘cold sores’), but can also cause genital herpes. HSV-2 is a sexually transmitted infection that causes genital herpes. Both HSV-1 and HSV-2 infections are lifelong.”
Wait, lifelong?
Yep. According to UVA Today, the virus never really goes away. “Instead, it lurks inside neurons, waiting for the right moment to strike again, a process known as reactivation.”
In this recent effort, researchers found that when neurons harboring the virus were exposed to stimuli that induce “neuronal hyperexcitation,” the virus senses this particular change and seizes its opportunity to reactivate. In other words, when the neurons flare up, so too does the herpes.
Their investigation took place at the University of Virginia’s Department of Microbiology, Immunology, and Cancer Biology (MIC). They discussed their discovery in their paper “Neuronal hyperexcitability is a DLK-dependent trigger of herpes simplex virus reactivation that can be induced by IL-1” published in the journal eLife.
Unsurprisingly, scientists are eager to learn more about the virus: the numbers of those who have contracted it are significant. As the authors explained in their paper:
“Herpes simplex virus-1 (HSV-1) is a ubiquitous human pathogen that is present in approximately 40–90% of the population worldwide (Arvin, 2007). HSV-1 persists for life in the form of a latent infection in neurons, with intermittent episodes of reactivation.”
Interestingly, the virus hijacks an immune response in the body. Per UVA Today:
“In response to prolonged periods of inflammation or stress, the immune system releases a cytokine, Interleukin 1 beta.” This cytokine is in epithelial cells in the skin and eye and is released when these cells are damaged by ultraviolet light. The researchers discovered that “Interleukin 1 beta then increases excitability in the affected neurons, “setting the stage for HSV to flare up.”
Their model was developed using mouse neurons infected with HSV. The paper’s authors noted why this focus on reactivation matters:
“Reactivation from a latent infection and subsequent replication of the virus can cause substantial disease including oral and genital ulcers, herpes keratitis, and encephalitis. In addition, multiple studies have linked persistent HSV-1 infection to the progression of Alzheimer’s disease (Itzhaki, 2018).”
In the bigger picture, too, the research highlights how “some viruses have evolved to take advantage of what should be part of our infection-fighting machinery,” concluded Anna Cliffe, one of the researchers.
Was this helpful?



