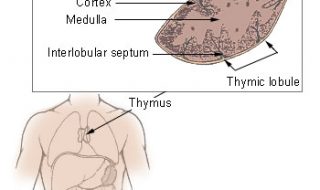
The thymus is one of those under appreciated organs you just don’t hear much about. Sitting in your chest, just in front of your heart, the thymus is at its largest and most active during infancy and childhood. By adulthood, the thymus has shrunk to practically nothing, being mostly replaced by fat. It plays an important role in the health of your immune system, and is the location where certain immune cells, called T-cells, go to mature and develop properly.
The thymus is like a schoolhouse for T-cells where they learn important lessons, like “recognize these sets of proteins as part of our own body and don’t attack them, but attack anything you don’t recognize because it must be a foreign intruder”. It allows the immune system to develop what is known as Central Tolerance. Without central tolerance, we develop auto-immune disease, which is essentially your immune system fighting a civil war against other parts of your own body. Diseases like Lupus, Type 1 diabetes, Myasthenia gravis, and many others are autoimmune diseases with the immune system actively damaging some parts of the body. In Type 1 diabetes, for instance, the immune system targets your pancreatic islet cells for destruction, resulting in loss of your bodies ability to make insulin.
It is also known that there are many varieties of T-cells, each with unique and important roles to play in immune function. One type of T-cell is known as the Regulatory T-cell or Treg. Tregs are special because they help to keep the other cells of the immune system from getting too wild and out of control (a recipe for autoimmune disease). They can go into an inflammatory situation where lots of immune cells are activated and ready to rumble, and tell those cells, “alright, everyone just calm down”, thereby suppressing the immune response. Some studies have show that Tregs can be infused into patients with autoimmune disease to help control their symptoms. They might even be a valuable way to suppress the immune system in people with an organ transplant, like a kidney or heart. Tregs are a way to use one part of the immune system to control other parts of the immune system – like fighting fire with fire – in the case of autoimmune disease.
These treatments, while promising, are still not fully evaluated and are not standard of care as of yet. One reason that not much research has been done using Tregs as a therapy is that they are hard to come by. They can be collected from the blood of donors, then grown in the lab to try to get enough cells for treatment, but the process is inefficient and doesn’t result in a large number of Treg cells.
This month in the American Journal of Transplantation, a team of Canadian researcher showed that discarded human thymuses are an excellent source of Tregs that can be harvested and used to treat a variety of immune mediated disease. So why would there ever be a discarded thymus? It turns out that when an infant is undergoing heart surgery, as might be done to correct a cardiac birth defect, the thymus is huge and in the surgeons’ way, and must be removed to gain access to the heart. This is true in infants where the thymus is very large compared to the heart, but not a problem in adults where the thymus has already atrophied to a tiny insignificant size.
Tregs can be identified and isolated based on unique protein markers on their cell surfaces such as CD25+,CD4+, and FOXP3. Other immune cells show different sets of markers making it possible to identify the different cell types, and select only the ones needed. The researchers found that they could identify and isolate many more Tregs from one discarded infant thymus, than could be generated from the blood of an adult donor. In fact, they could show that there are more Tregs in an infant thymus than are present in the entire circulation of an adult. They also found that the Tregs from discarded infant thymus function better compared to those recovered from the process of blood donation. It is thought that this might be due to the immaturity of Tregs coming from thymus versus blood, since those in the blood have been around longer and show other markers of cellular aging, such as shorter telomere length.
Perhaps if more Tregs become available from thymus harvesting, more clinical studies studies will be conducted that may hopefully find effective ways to treat autoimmune diseases that today are very difficult to control and create much suffering in the lives of so many people.
Reference Article:
1. Am J Transplant. 2016 Jan;16(1):58-71. doi: 10.1111/ajt.13456. Epub 2015 Sep 28. Discarded Human Thymus Is a Novel Source of Stable and Long-Lived Therapeutic Regulatory T Cells.
Dijke IE1,2, Hoeppli RE3, Ellis T1,2, Pearcey J1,2, Huang Q3, McMurchy AN3, Boer K4, Peeters AM4, Aubert G5, Larsen I1,2, Ross DB2,6, Rebeyka I2,6, Campbell A3, Baan CC4, Levings MK3, West LJ1,2,6.
Was this helpful?



