Three babies aged six to eighteen months suffering from an incurable breathing condition were saved by doctors who printed a 3-D implant. The implant is made out of a special biodegradable plastic that dissolves in three years (just enough incidentally for kids to be out of harms way permanently). It’s also designed to grow and expand as the babies age, hence it’s called a 4-D printed implant since time is considered an additional dimension, in this case.
The kids were suffering from a severe form of tracheobronchomalacia, which affects about 1 in 2,000 children around the world. The disease regularly causes the windpipe to collapse, blocking breathing. There is no cure for the disease, and the children in question had a life expectancy estimated at days to weeks. Prior to surgery, the children had tubes attached to their necks and were placed in a permanently ventilated enclosure. At times, the babies suffered severe complications and had to be resuscitated.
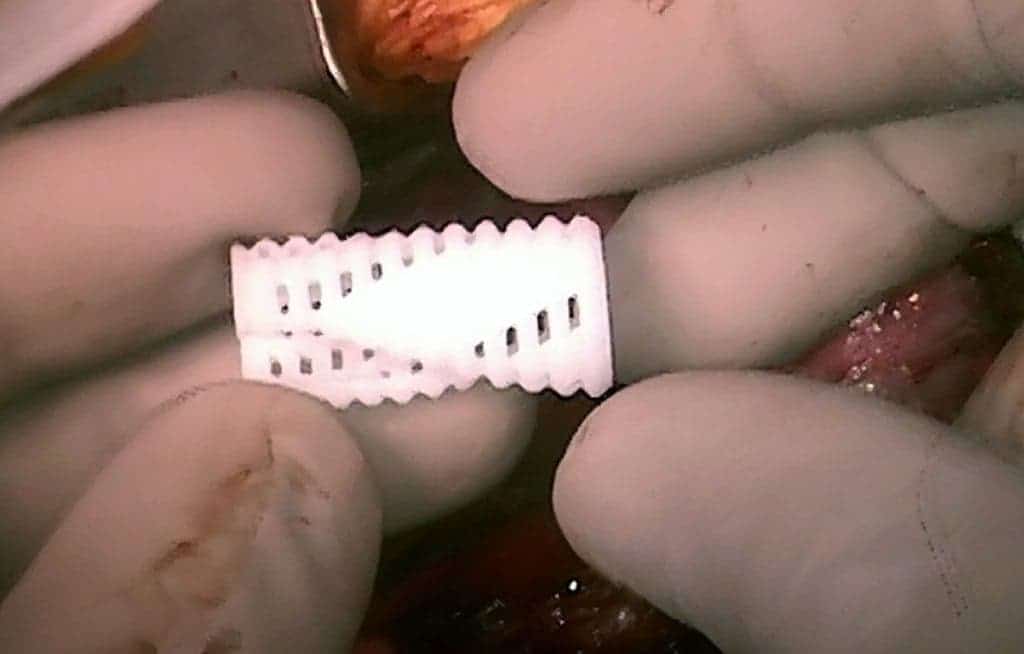
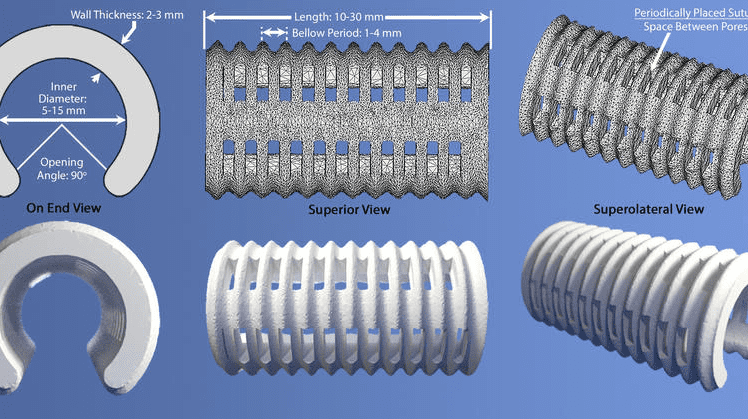
Their lives was saved however by a tiny white tube no thicker than a pencil’s lead. To make the implant, the team at Michigan’s C.S. Mott Children’s Hospital first made CT scans of the babies’ necks to build a model of the collapsed airways. Then a computer program used this geometry to design a 3-D model of the splint which would expand the airway and allow normal breathing. It was only a matter of printing the implant, using a laser 3-D printer which deposits polycaprolactone. So, every implant was custom made to fit inside the baby’s necks perfectly. Each for $10 and a couple of hours of design work.
“This is the first 3D-printed implant specifically designed to change shape over time, the fourth dimension, to allow for a child’s growth,” Dr. Glenn Green, associate professor of pediatric otolaryngology at C.S. Mott Children’s Hospital in Michigan.
“Holidays are not spent in the hospital anymore,” Green said. “Instead of lying flat on their backs for weeks on end, these children are learning to sit and stand and run.”
“I honestly don’t think we can ever thank Dr. Green and his team in Michigan enough,” Natalie Peterson, mother of sixteen-month-old Garrett Peterson, said. “We know that without this procedure, Garrett was a month or so from passing away.”
If children survive past age three, they’ll eventually get strong enough to get rid of tracheobronchomalacia with no sign they ever had the disease which nearly wiped them out as newborns.
“We were honestly terrified, just hoping that we were making the right decision,” the mother of five-month-old Ian Orbich , Meghan Orbich, said in a statement. “I am thankful every single day that this splint was developed. It has meant our son’s life. I am certain that if we hadn’t had the opportunity to bring Ian to Mott, he would not be here with us today.”
Their work was described in a paper published in the journal Science Translational Medicine.
Was this helpful?



